Technology
Additive Manufacturing
Since 2014, our conventional manufacturing processes (such as casting and machining) have been supplemented by additive manufacturing technology. This is one of the most innovative advances of the 21st century and allows the manufacture of components with extremely complex structures and geometries which could never be reliably or efficiently produced via conventional methods. When used in conjunction with scan data for an individual patient, additive manufacturing can be used to produce an implant which precisely fits the anatomy of the patient or which precisely fills a bony defect within a patient. Additionally, this technology can markedly accelerate manufacturing time (especially for individualised prostheses), offer a high degree of design freedom and enable the incorporation of structures which provide high degrees of primary stability and secondary fixation to bone.
The process of additive manufacturing – electron beam melting (EBM)
Firstly the structure and geometry of the proposed implant component is defined electronically. Usually this involves combining 3D data from a patient scan with a design engineer’s input and a surgeon’s input. In essence this information is then used to direct an electron beam inside a chamber containing small amounts of titanium alloy (TiAl6V4) powder. Each time the electron beam is fired it causes the selective melting of the powder and the design materializes 50 μm layer by 50 μm layer until it is complete.

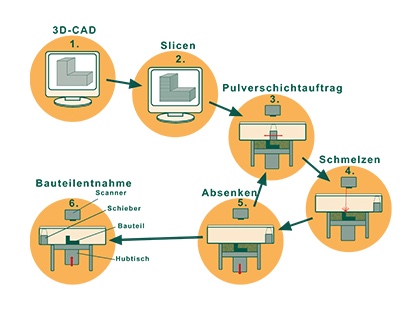
1. 3D-CAD
The component to be produced is constructed three-dimensionally on a PC and represents the starting point of manufacturing.
2. SLICING
The model is virtually cut into individual slices, each of which corresponds to the layer thickness of the additive manufacturing.
3. POWDER APPLICATION
In this, the first physical step, an even powder layer is applied using a blade system. The height of the powder layer corresponds to the slice thickness previously generated at the PC and is in the order of 50μm.
4. MELTING
Using an electron beam, the powder is exposed according to pre-defined paths. The melt solidifies and forms a solid melt-metallurgical construct. During subsequent cycles the same process is applied completely fusing the most recent layer or slice with those underlying it formed during previous cycles.
5. LOWERING
After the formation of each layer the working platform is lowered by the layer height. Then the cyclic processes described in steps 3 to 5 can be repeated until the design has, quite literally, materialised.
6. COMPONENT REMOVAL
The components are removed and all non-exposed powder is recycled and used for subsequent designs.
EPORE®
These titanium alloy (TiAl6V4) components are made via our additive manufacturing process hence the ingrowth surfaces are in every way an integral part of the implant itself - and hence should not be viewed as coatings. The ingrowth surfaces on EPORE® devices are typically characterised by rods of 330μm to 390μm in diameter giving them a low modulus of elasticity (similar to that of bone) and a high porosity (also similar to that of bone) so as to encourage bony ingrowth and long term fixation. EPORE® implants are available for a variety of standard applications and can also be custom made for individual patients. Furthermore because titanium alloy is a biologically inert material which is also ductile and corrosion resistant with a high fatigue strength, EPORE® implants are particularly well suited to meet the demands they will be subjected to in vivo.

mechanical properties in comparison
EPORE®
- porosity 60 %
- rod thickness 330 to 390 μm
- modulus of elasticity 3 GPa
Cancellous bone
- porosity 30 to 90%
- trabecular diameter 0.1 to 0.2mm
- modulus of elasticity 0.5 to 1.5 GPa